Three years ago I was standing in line in a bank in Costa Rica to exchange money while on a much needed vacation. My vision suddenly got blurry, sounds became distant, and everything started spinning.
Next thing I knew I woke up lying on the marble floor of the bank with my partner shouting my name at me, and two Costa Rican ladies had my legs tossed over their shoulders as if they were helping me give birth. They were shouting at me in Spanish, which I don’t understand, but their faces looked very concerned.
But it wasn’t until after I returned to the States that things got weird. I fainted twice that day in Costa Rica and had a fever the rest of the trip. In the following weeks and months, new and confusing symptoms arose, each one piling on top of the previous list of misery. I kept nearly fainting, the fever persisted, and muscles all over my body started twitching, sometimes strong enough to wake me from sleep.
I became so weak that I literally had to crawl upstairs, I felt sudden stabs of pain so sharp that I thought I was being stung by a hornet or stepping on a nail, my joints hurt like arthritis, but the pain kept moving. My skin hurt. Every time I ate, I’d start to faint and only come to as my head was about to hit the plate. Scary and violent images flashed through my mind. My heart rate would often beat as high as 140 while I was just standing stationary.
I was so confused that some days I could not figure out how to cross the road, and something was so wrong with my muscles that I couldn’t make them work unless I concentrated. One day I suddenly lost vision in my eye. My heart beat so abnormally that I went to bed many nights certain that I’d die from a cardiac problem before morning. When I did wake up, I was immediately aware of this deep heaviness that invaded all of my muscles, obvious before I even moved in the morning. For nine months I woke up each morning hoping that the heaviness was gone, disappointed when it was still there—often also disappointed that my heart had not given out in the night.
Of course I went to many doctors during this time. Test results were frustratingly normal, except for a possible current, recent, or past mono infection. My doctor therefore concluded that it was mono and told me to wait it out. However, after six months of waiting for the “mono” to resolve, while symptoms continued to worsen, my doctor concluded, “You now have post-viral fatigue. I can do nothing for you, except help you fill out disability papers.”
Turning Point
I felt lost, abandoned, helpless, unwilling to continue living as I was but unable to fix it. Out of desperation I made an appointment with a doctor in private practice that specialized in Integrative Medicine. He listened to me for two hours as I cataloged the scope of the illness. It was a relief to me to at least have a medical professional listen to my story and take it seriously.
At the end of the appointment, he stated that he wanted to run a Lyme Disease test. I explained that I had been tested for Lyme early in the illness and that it had come back negative. He explained that the current state of Lyme testing is terrible and that the tests often produce false negatives. The test relies on measuring antibody response to the Lyme infection, but Lyme inhibits the body’s ability to produce those antibodies. In addition, the current testing and treatment guidelines for Lyme appear to be more informed by opinion and politics than by good science, so the best path to diagnosis is through good clinical interviewing. Finally, he explained that a high percentage of ticks in Wisconsin carry infections other than Lyme, and these infections can also make a person very sick. I had never been tested for any of these other infections.
Weeks later I was surprised to learn that I was positive for an active Lyme infection. Subsequent testing also showed that I was positive for active Bartonella, Rocky Mountain Spotted Fever, and Babesia infections.
Living with Lyme
In contrast to what many have heard, Lyme Disease is not an easy infection to treat, especially if it is advanced, or if there are co-infections. Treatment has been long, brutal, expensive, heart wrenching, confusing, and very isolating. After more than two years of treatment, my health remains quite fragile, although it is significantly improved from where it was prior to treatment. I was only recently able to return to work full-time, and I still have plenty of bad days. Relapses seem to be a part of this constellation of infections, so I live with the knowledge that I could return to that hell at any moment.
Although I am still too close to these events to fully process them, I have learned a few key things in the past three years.
To everybody, whatever your current level of health, find a way to get the most life out of what you’ve got. I promise you, things can get much, much worse and with lightning speed. I will probably never get to go on those backpacking trips I had planned, or rehab a house, or sail the Pacific. I grieve the loss of those possibilities. I also do not know if the health I’ve got will hold, so I need to carve that paddle, explore local wetlands, and cook some new dishes while I can.
If you struggle with ill health, my heart goes out to you. Work hard to find the balance between acceptance of what you’ve got and refusal to give up. That’s a really hard balance to find. If you’ve been through some sort of serious illness, you already know that some people will really step up in amazing ways, while others will deeply disappoint you. That is a part of this journey. Be open to allowing those who step up to do what they are good at, and try not to spend energy on resenting those who have let you down.
Take Care of You
Serious illness is inherently selfish. That’s OK, but be nice and say “please” and “thank you” even when you don’t feel like it. An attitude of gratitude toward those who are helping you will go a long way in helping them to endure in the long run. Be flexible. If you are no longer able to do the things you love, find new things to love. I used to love backpacking and mountain biking. Because I can no longer do that, I have taken up paddling. Although my old self would want to circumnavigate Lake Superior, my new goal is to someday circumnavigate Lake Wingra. On days that I am too weak to paddle, I watch cooking shows to learn new approaches to food. When I can stand, I am learning to enjoy Tai Chi.
If you currently have reasonable health, please don’t waste it! Do the things you love, and take care of your body. Healthy people say a lot of stupid things to those who have some kind of illness. Please do not ever say to someone who is ill, “You look great,” or, “But you don’t look sick,” or, “Don’t worry, you are going to be fine.” Those are probably some of the most dismissive things you can say, and they feel isolating to the person hearing them. Deal with your own discomfort with illness elsewhere, and don’t try to fix the fact that your friend feels bad by denying it. You can say, “How are you doing?” or “I want to help; what would feel supportive to you?” Even better, offer something specific like, “Can I come over and mow your lawn?” In my three years of often disabling illness, there have only been three people who offered specific help, and I still cry with gratitude when I think of them. Do not offer treatment advice unless you are asked, even if you would prefer they choose a different path. Your job is to support them through their journey; their treatment decisions are between the person and their chosen health care provider.
Seek to Support
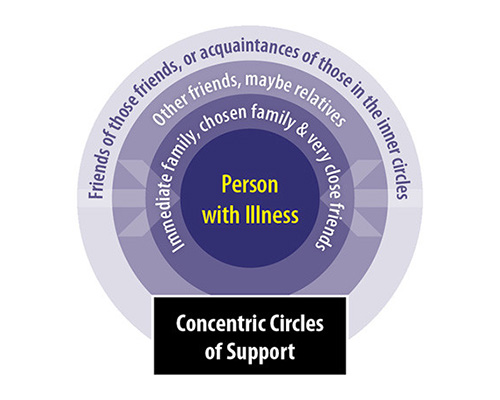
Finally, I want to share a model I call the Concentric Circles of Support that I learned from an area therapist. In the middle is the person with the illness. In the next circle are those who are closest to that person. It may be immediate family, or maybe more often with LGBTQ folks, chosen family and very close friends. The next circle contains other friends, maybe relatives. The next circle contains friends of those friends, or acquaintances of those in the inner circles. The key to this model is that all support goes in an inward direction and never outward. The acquaintances support the friends who support the close friends who support the person with the illness. Never the other way around! Some of the most stressful situations I’ve seen are when this rule is broken. For example, a mother who is supporting a child with cancer and who is being asked for information, advice, and support from a relative will be extra stressed because the rules of this model are being broken. The relative must only provide support to the mother who is supporting the ill child.
I rarely look at photos from that trip to Costa Rica. They are too painful. I see over-the-top joy on my face in pictures of me white water rafting, knowing that 48 hours later I came to on the marble floor of that bank. Core aspects of Me were permanently taken away through no fault of my own. In addition to continuing to fight for whatever level of health I’m able to attain, my task for the future has to include getting to know this new Me and coming up with a new bucket list because I’m not capable of most of the things on my old list.
If you or someone you love is in a similar situation, persevere. Don’t give up. Cry when you need to, and keep moving forward in the way that best works for you.
Sue Gill and her partner, Sheri, have lived in Madison since 2000. They keep busy with their two dogs, Frankie and Maslow. Sue is a psychologist in private practice and can be found at madisontherapy.com.






















0 Comments